What Is Somatic Experiencing? A Nervous System Approach to Trauma Healing
What Is Somatic Experiencing (SE)?
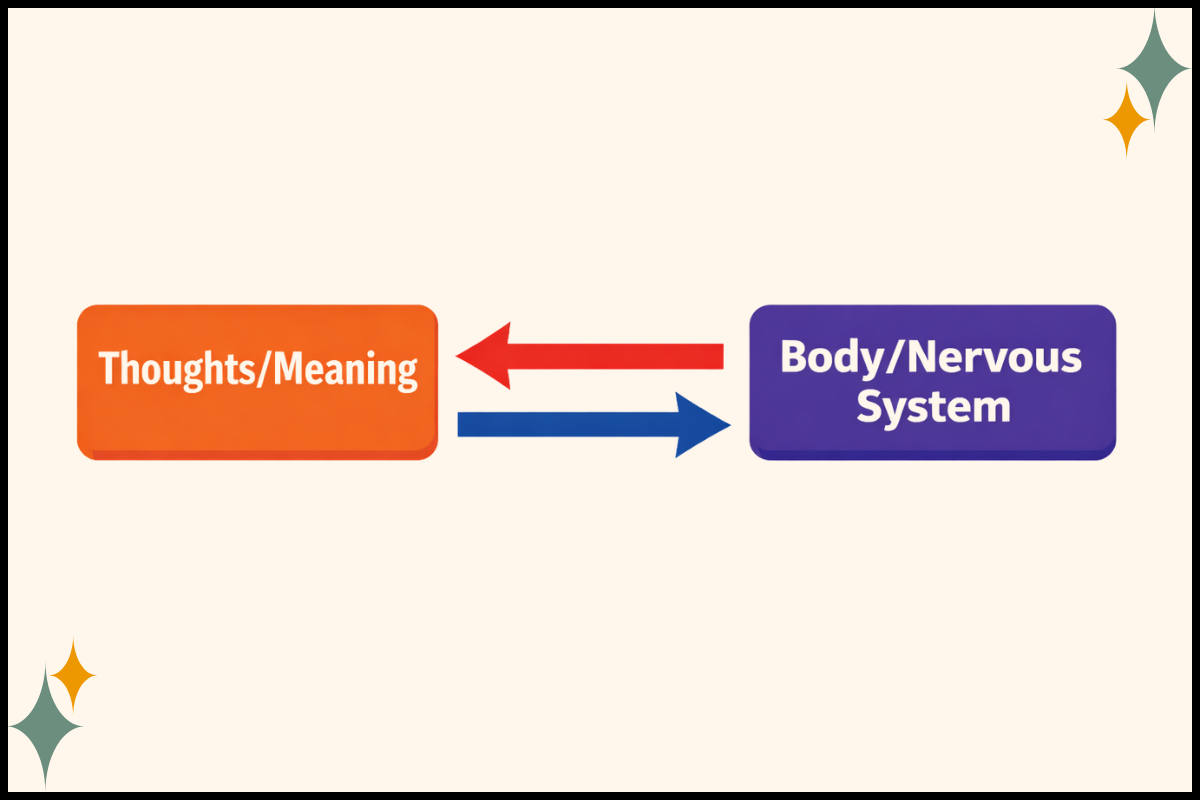
Somatic Experiencing (SE) is a nervous system–centered trauma model that helps people track sensations and nervous system shifts in small, manageable steps so the body can move out of survival mode.
Clinically, I think about SE as a way of working with the state a client is in, not only the story they can tell. It’s built to meet the reality most of us see every week: a client can understand what happened, make meaning of it, even talk about it clearly, and their body still reacts like the threat is present.
SE was developed by Dr. Peter Levine. It’s influenced by trauma physiology research and the way protective responses (fight/flight/freeze/collapse) can get stuck or incomplete after overwhelming stress. Levine’s book Waking the Tiger helped bring these ideas into wider public awareness.
Why Insight Alone Isn’t Always Enough
This is where trauma therapists often feel quietly defeated.
We do solid work. We build safety. We track patterns. We help clients name distortions, make sense of trauma responses, and hold nuance.
And still… a client walks out of session and their body does what it does: bracing, scanning, collapsing, panicking, disappearing.
The line I hear (and have said myself in consultation) is some version of “I know all the things we’ve worked on, but I just can’t feel them.”
SE gives us a framework for that gap. Not a “fix” or magic lever but a way of understanding what’s happening without blaming the client or assuming the therapy is failing.
As a therapist, this is also where SE hits me.
Because when insight isn’t moving the needle, my nervous system wants to do something right now! I want things to go faster, or I think I have to work harder than my client. That can look like talking more or searching for the “perfect” intervention so I can solve everything.
SE approaches these stuck points by asking a different question: What happens if the nervous system sets the pace?
That question can be relieving and it can also be maddening (for both your client and you!) 😅
Core Principles of Somatic Experiencing
Trauma Is a Biological Response Not a Character Flaw
SE takes trauma responses seriously as biology and the body’s natural survival response of fight/flight/freeze/flop and even fawn.
When those protective responses don’t fully “finish,” after a traumatic event the nervous system can stay stuck in danger mode even when danger is over.
And that’s the part that can look confusing from the outside.
The client who “has it all together” and still can’t sleep
The client who understands their triggers and still goes numb
The client who has years of therapy and still feels trapped in their body
From an SE lens, those aren’t failures. They’re protective strategies with momentum.
Titration: Why SE Works in Small Doses
Titration is one of the most therapist-friendly parts of SE, because it gives us permission to stop trying to do “the whole thing” in one session.
Titration means working in manageable increments so the client stays within their capacity or window of tolerance. When we go beyond capacity, we can get flooding, dissociation, collapse, shame spirals, and that familiar feeling of, “I made it worse.”
Titration is pacing with intention, it’s the opposite of white-knuckling.
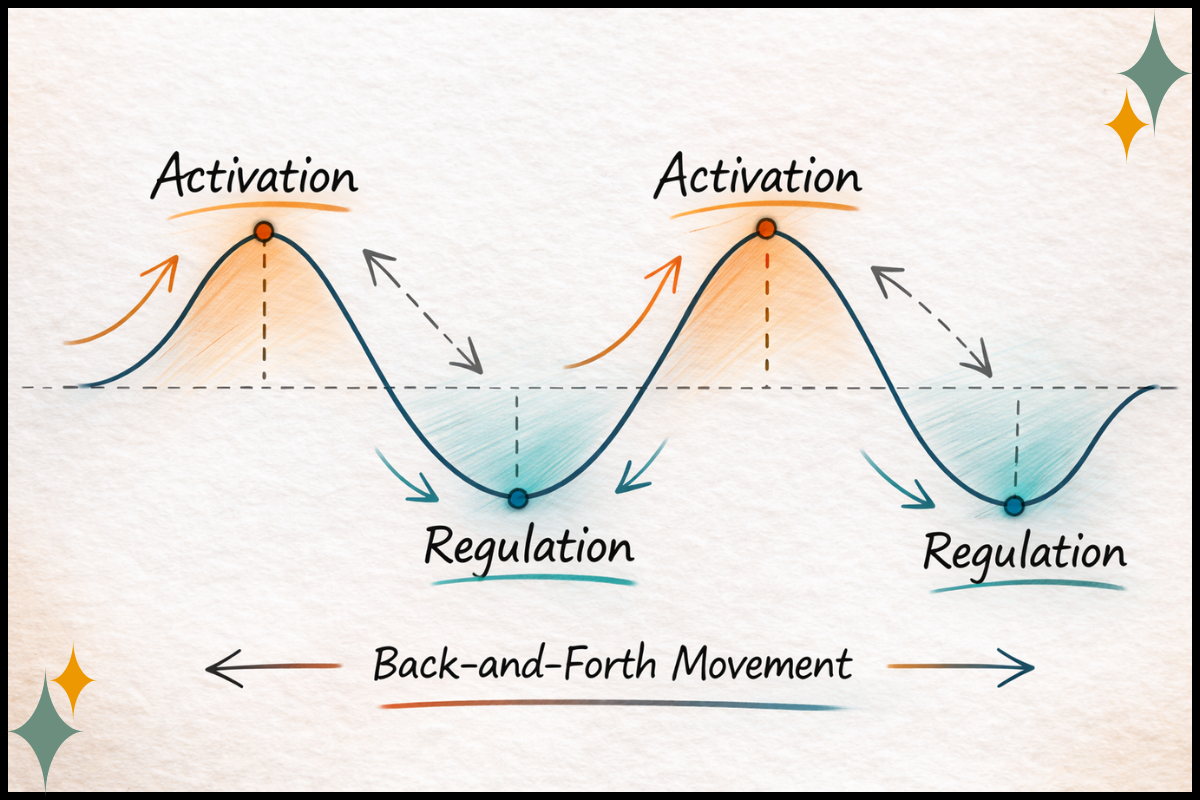
Pendulation: Moving Between Activation and Regulation
Pendulation is the movement between activation and regulation. Safety and intensity. Edge and resource.
In real session language, it sounds like:
“Let’s notice that tightness for a moment… and now look around the room.”
“Can we touch the fear for two seconds… and come back to your feet on the floor?”
“Let’s find what feels steady before we go any further.”
This back-and-forth helps the nervous system learn, “I can move through this and come back.”
That learning matters.
What Happens in a Somatic Experiencing Session?
Slowing Down the Trauma Narrative
SE sessions often reduce the pressure to tell the full story. Many clients feel relieved by that and many therapists do too (once we trust the process 😉).
In practice, this can look a lot like -
Less: “Start at the beginning and tell me everything.”
More: “Notice what is happening right now as you say that.”
This doesn’t remove meaning-making, in fact it can actually deepen it in many ways. It does, though, change the timing because we’re first working with the nervous system so that the story can land in a body that has more capacity.
Tracking Sensation Instead of Retelling the Story
Because we’re focusing on increasing capacity in the body instead of retelling the story, SE tends to use questions that sound almost too simple, until you watch what they do in the room:
“What do you notice in your body right now?”
“Where do you feel that?”
“Get curious about what happens if we stay with that for a few seconds?”
“Can we find one place inside that feels even just a little bit calm, neutral, or grounded?”
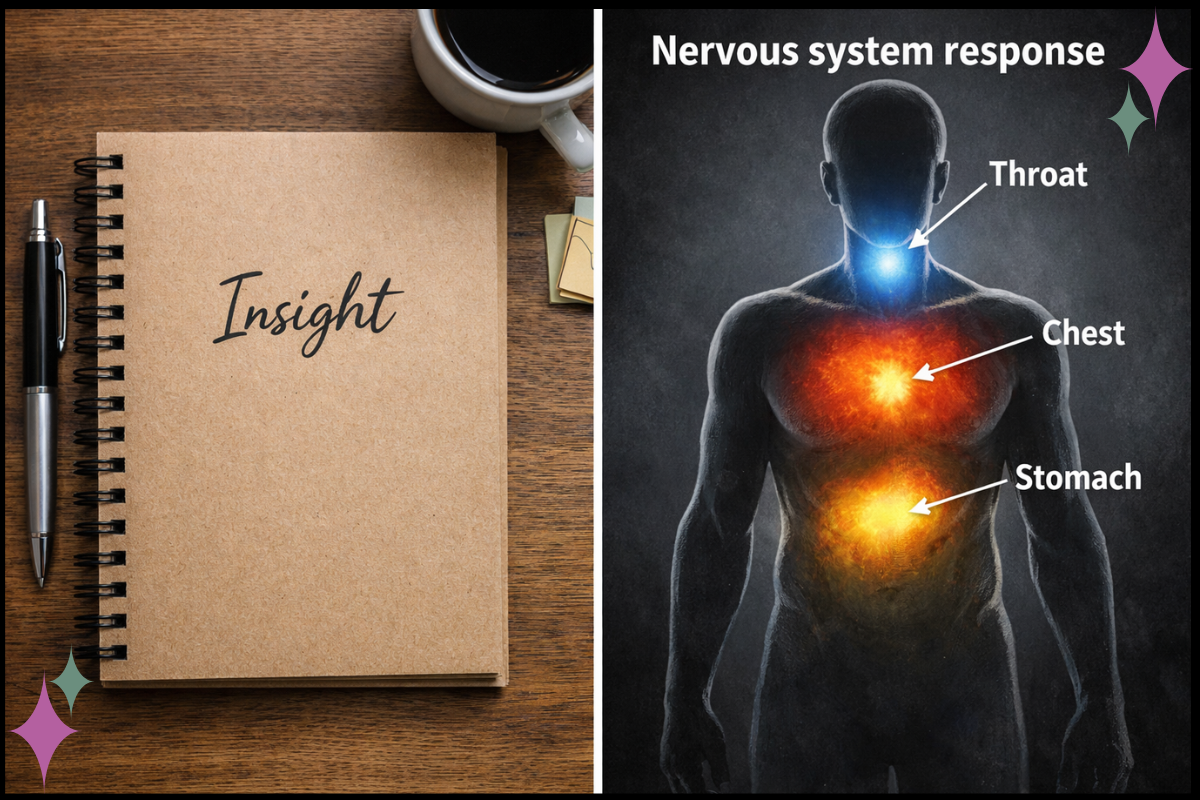
In responding to these questions, clients might share that they’re feeling tightness, buzzing, heaviness, numbness, heat, nausea, a push/pull impulse, a change in breath, a shift in posture.
For therapists, this is where SE can feel unfamiliar at first. Many of us were trained to privilege narrative and cognition. Sensation tracking asks us to listen to a different channel.
The Goal of SE Is Not Tolerance, It’s Nervous System Updating
This is the line I want trauma therapists to keep close.
The goal of somatic experiencing isn’t building a client who can tolerate more pain.
The goal is helping the nervous system update so pain doesn’t keep announcing danger in the present. That’s the difference between a client feeling distress and a client getting hijacked by distress. When the nervous system can register, “This is uncomfortable, but not unsafe,” they recover faster, they don’t spiral as hard, and sessions stop costing them the rest of the day/ life.
Common Misconceptions About Somatic Experiencing
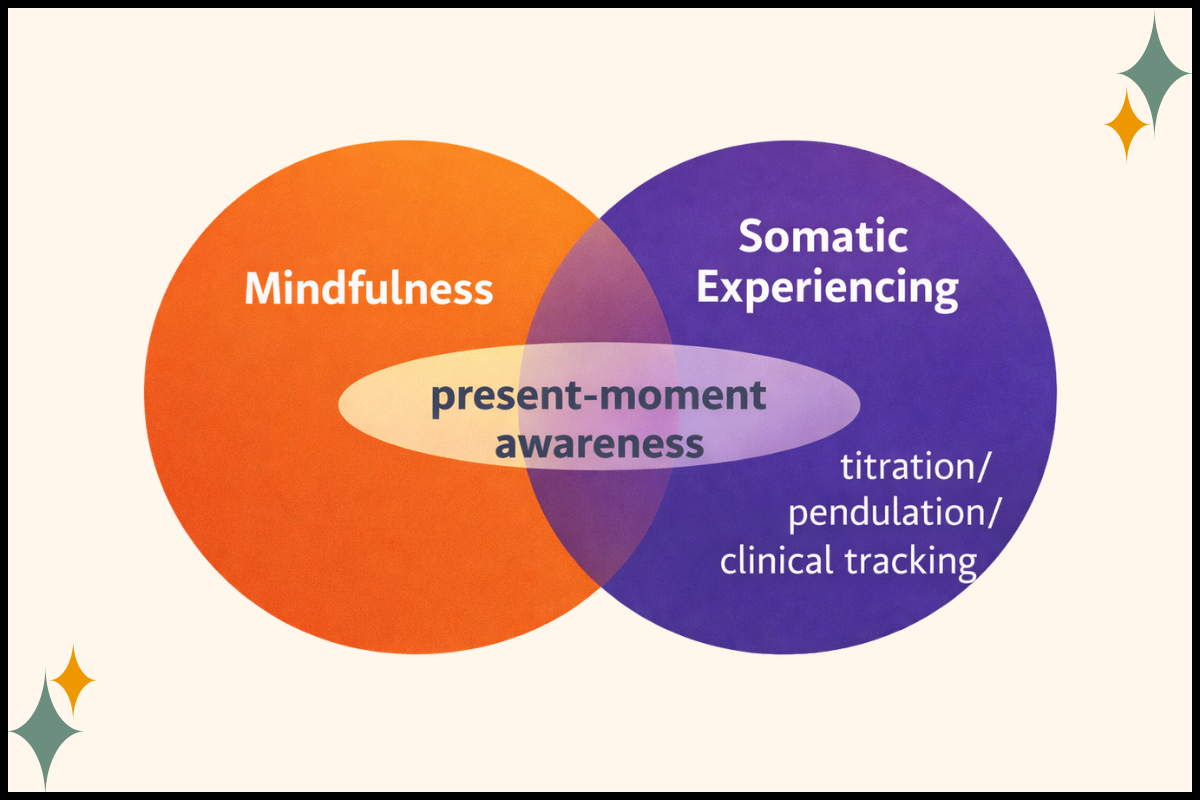
Is SE Just Mindfulness?
SE can include mindful awareness, sure. The difference is structure and clinical intent.
Mindfulness can help someone notice what’s happening. SE focuses on what the nervous system does with that information, moment by moment, with pacing, containment, and tracking.
Will Paying Attention to My Body Make Things Worse?
This fear is valid because many trauma survivors learned that body awareness ramps things up fast.
SE is designed around pacing for that reason (that’s where titration and pendulation come in). The work stays below overwhelm and includes resourcing, orienting, and coming back to the room.
From a therapist standpoint, this is where your steadiness matters. Your pacing matters. Your ability to slow down even when you want progress matters.
If We’re Not Talking About the Trauma, Are We Avoiding It?
SE isn’t about avoidance. It’s discernment.
Sometimes the most helpful work is getting the nervous system oriented to the present before touching the past. When we force the story without capacity, we can get reactivation instead of integration.
Who Is Somatic Experiencing a Good Fit For?
Somatic Experiencing therapy can fit well for clients who say:
“I understand it, but my body won’t cooperate.”
“My symptoms feel physical.”
“I go numb, shut down, or panic even when I know I’m safe.”
It can be useful with panic, dissociation, shutdown, chronic bracing, startle, sleep disruption, and other body-based patterns that keep showing up.
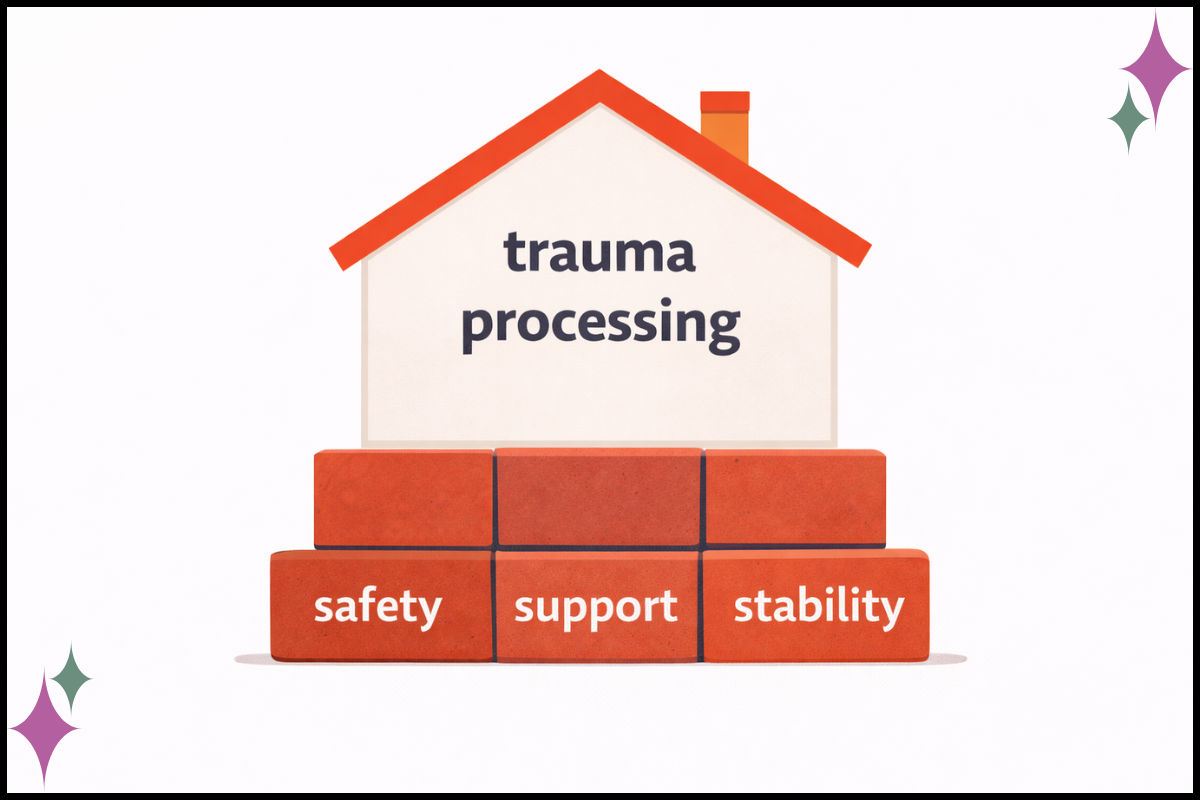
When Stabilization May Come First
When working with SE, timing matters.
If there’s ongoing threat, environmental instability, severe dissociation, or very limited support outside the session, the client’s stability may need to come first. That doesn’t mean “no SE.” It means the work needs a steadier foundation.
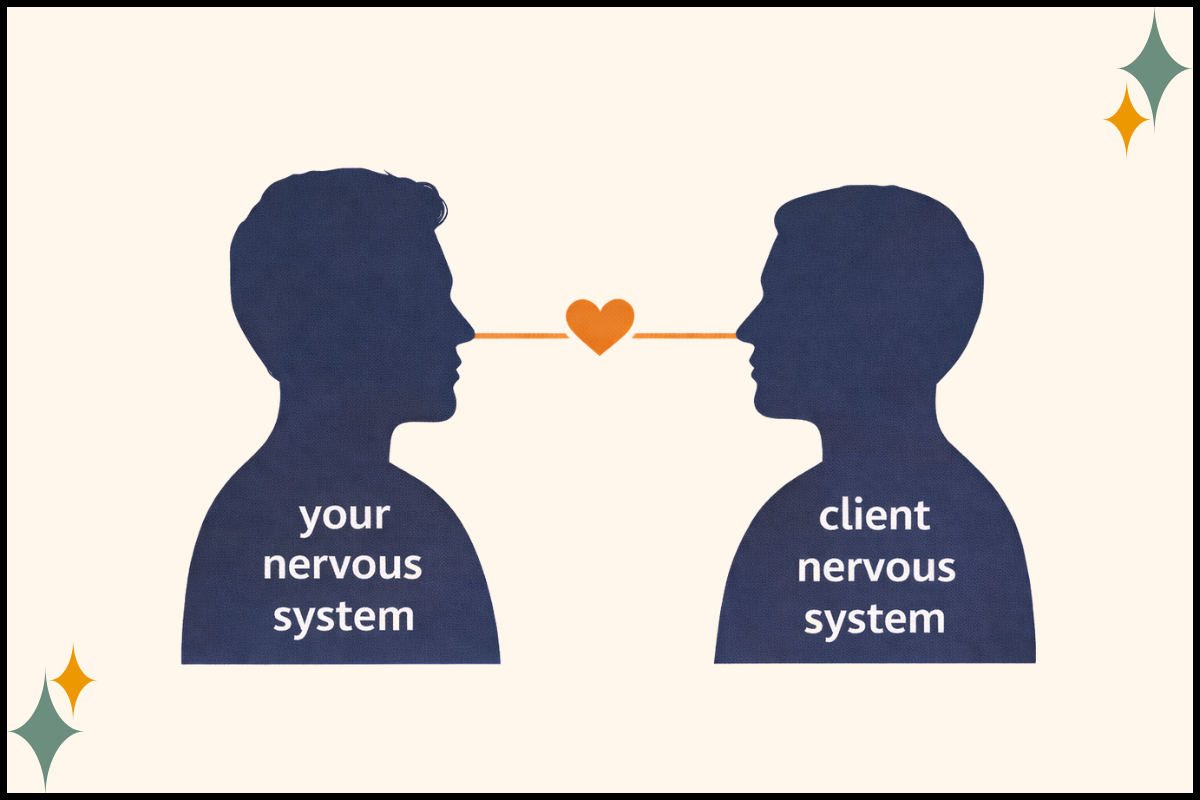
What Somatic Experiencing Requires From the Therapist
Somatic Experiencing asks you to track your own urgency, especially that subtle “fix-it” energy that can arise in your body when a client begins to slow down. It invites you to notice the impulse to speed things up and move the process forward when the space feels uncertain or quiet. It also asks you to gently turn toward the fears underneath that urgency, including the fear of doing harm, the fear of looking incompetent, and even the deep desire to do good, meaningful work, and to hold all of that with the same curiosity and regulation you offer your clients.
SE can bring up a lot of of performance pressure for trauma therapists, like
“I have to be perfectly regulated to do this right.”
“I’m not doing enough.”
Nope.
Your nervous system matters, and you’re still a human with a nervous system. The work is noticing what happens in you and staying honest about it, so you can keep choosing pacing and attunement.
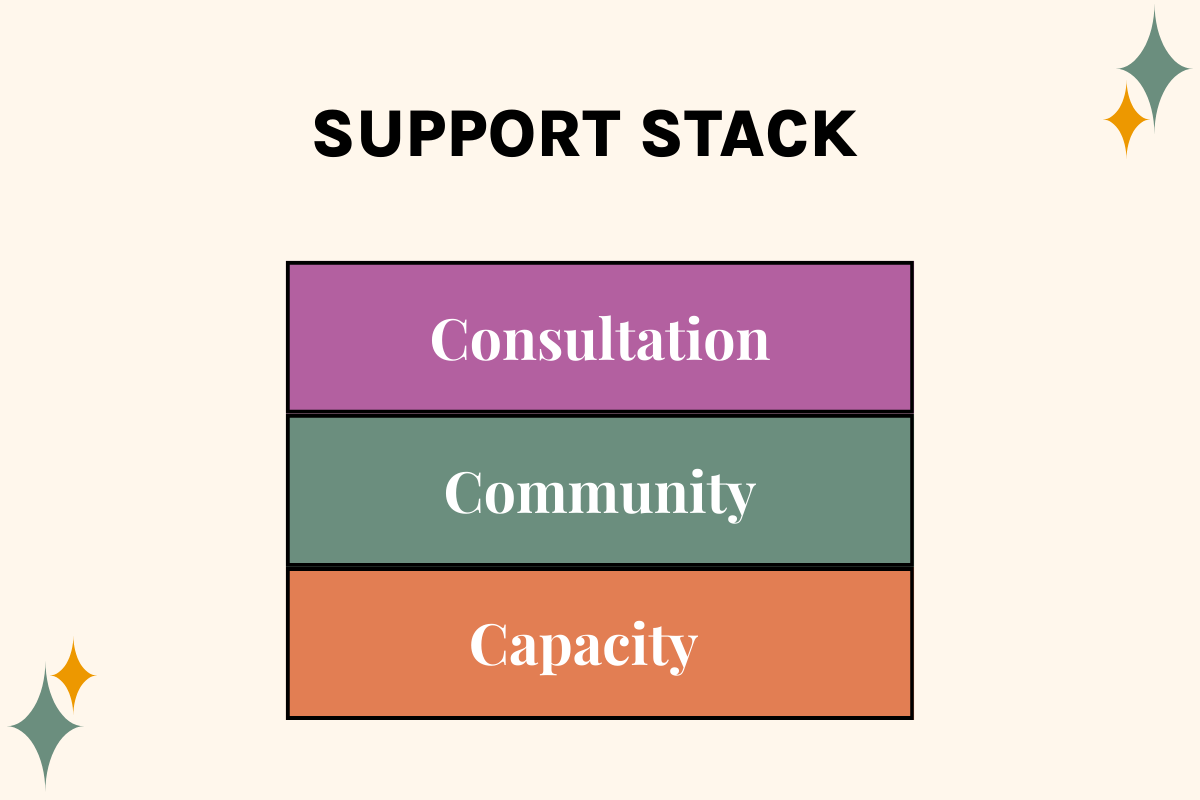
Why Consultation and Community Matter in Somatic Work
Somatic Experiencing can be super powerful in trauma work. It can also be tender, slow, and easy to second-guess.
This is why trauma therapists need places where the question isn’t only “What intervention did you use?” but “What was it like to be in the room?” and “What did your body do while you were holding that?”
That’s the kind of support that protects your longevity in this work. It’s part of why I built The BRAVE Trauma Therapist Collective: not to hype training, but to give trauma therapists a place to be human with other trauma therapists who get what this work asks of therapists.
Is Somatic Experiencing Right for You?
If you’re a client reading this: you don’t have to decide today. You’re allowed to ask questions, interview therapists, and choose pacing that respects your body.
If you’re a trauma therapist and you’re feeling drawn to SE, I don’t think the first question is whether you’re “good enough” to do it. I think the first question is whether you have the kind of support SE assumes: pacing, consultation, and a place to process the nervous system load of this work.
Because SE isn’t just a set of tools. It’s a way of being in the room, and it asks something of your nervous system.
If you’re realizing you’ve been doing all that work alone, you’re not the problem. You’re just doing trauma therapy inside a system that normalizes isolation.
And that’s the gap BRAVE exists to meet.